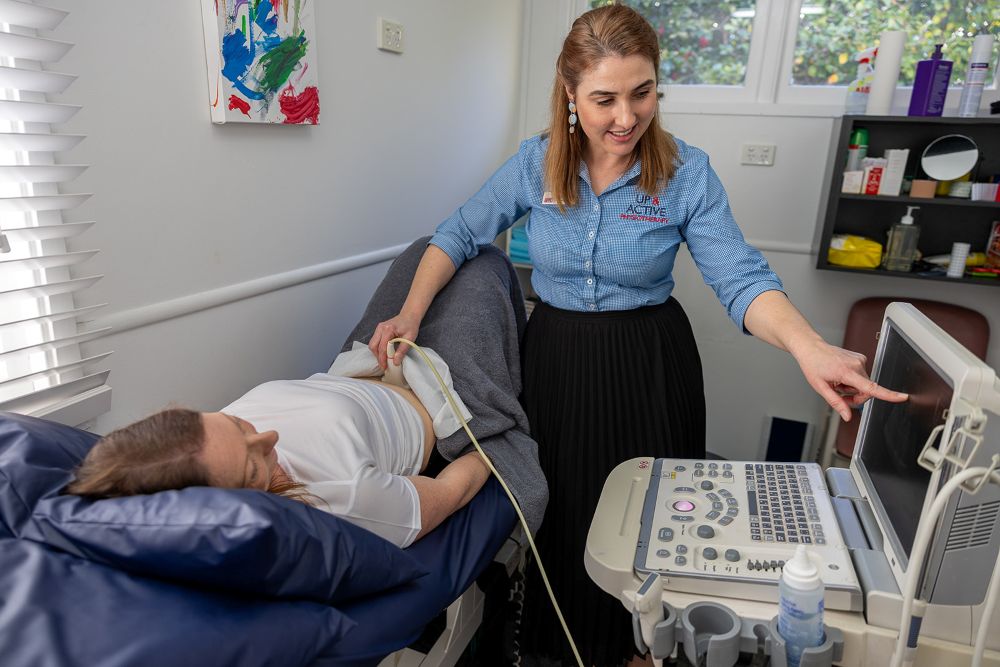
Pelvic Health Physiotherapy
Pelvic Health Physiotherapists treat pain and medical conditions related to the pelvis. This includes continence, urinary and anorectal symptoms, women’s health, pregnancy and pessary fittings.
At Up and Active all genders are welcome and we treat all ages, including children from four years. Pelvic Health Physiotherapists treat pain and medical conditions related to the pelvis. This includes continence, urinary and anorectal symptoms, women’s health, pregnancy and pessary fittings
Pelvic Health physiotherapists often co-treat with medical doctors or other allied health professionals including dietitians, psychologists and musculoskeletal physiotherapists. We are in regular communication with local GPs, obstetricians, gynaecologists, colorectal surgeons, gastroenterologists and urologists for a team approach to your care.
PHYSIOTHERAPY
PELVIC HEALTH PHYSIOTHERAPY
Oncology Physiotherapy
LYMPHOEDEMA
EXERCISE PHYSIOLOGY
HOME VISITS
CORPORATE ASSESSMENTS
Conditions Treated By Our Pelvic Health Physiotherapists

Urinary Symptoms
Urinary frequency: going too little or too frequently to the toilet can be bothersome and problematic. Clinically reasoning through history taking and bladder diary analysis can help to identify contributing factors and treatment options.
Voiding symptoms include hesitancy, slow stream, straining to pass urine, pain to pass urine, sense of incomplete emptying, dribbling urine after already dressed and double voiding. Presence of these symptoms can often indicate that something else is going on, such as prolapse or overactive pelvic floor muscles.
Storage symptoms include absent, reduced, increased or urgent bladder sensation of filling. An ultrasound and bladder diary is often required to determine appropriate conservative treatment options, or whether referral on to a Urologist and/or Gynaecologist is indicated.
UUI: Urge urinary incontinence (UUI) is urinary incontinence preceded by a sudden and strong need to urinate (definition provided by Australian Commission on Safety & Quality in Health Care). There are often clues in a good history taking, as well as a completed bladder diary that helps us decide contributing factors and tailor treatment choices
SUI: Stress Urinary Incontinence (SUI) is the leaking of urine during activities that increase pressure inside the abdomen and push down on the bladder, such as coughing, sneezing, running, or heavy lifting (definition provided by Australian Commission on Safety & Quality in Health Care). There can be many contributing factors to this condition, such as weak pelvic floor muscles and tissue changes during menopause. Pelvic health Physiotherapists aim to identify all the contributing factors to facilitate targeted treatments.
Bedwetting (Nocturnal enuresis): a common childhood condition, management options from 7years old
Coital incontinence; can be due to an overactive bladder or stress urinary incontinence. Adequate assessment and treatment can resolve this issue

Prolapse
The pelvic organs include your bladder, womb (if assigned female at birth) and rectum. Pelvic organ prolapse occurs when one or more of these organs bulges against, or sags down into the vagina and the muscles and ligaments in the pelvic floor become stretched, or too weak to hold the organs in the correct place (definition provided by Australian Commission on Safety & Quality in Health Care).
Symptoms you might experience:
- Pressure or bulging in your vagina, often made worse with physical activities
- Painful intercourse, or less sensation with intercourse
- Less control with your bladder or bowels
- Urinary problems such as retention (unable to urinate when your bladder is full), incontinence, and urinary tract infection
Pelvic health physios can determine the contributing factors and provide treatment options relevant to your type/s of prolapse. These may include pelvic floor muscle training and a pessary.
Anorectal Symptoms
- Constipation – this can be a tricky diagnosis. Many people believe they are not constipated when in fact they may be. Physiotherapy can assist in an accurate diagnosis and provide effective treatment options in conjunction with your GP and/or Gastroenterologist and/or Colorectal specialist
- Incomplete evacuation (a sense that not all the bowel motion has passed)
- Straining
- Faecal and/or flatal incontinence (the involuntary loss of stool or wind from the back passage). There are different types of faecal/flatal incontinence – and a thorough assessment provides insight into the driving factors to facilitate targeted treatment options.

Persistent Pelvic Pain
Persistent pelvic pain is complex and often multi-factorial in nature. Endometriosis is a common condition where persistent pelvic pain is often prevalent. However, not all people with persistent pelvic pain have Endometriosis. Bladder Pain Syndrome / Interstitial Cystitis and Coccyx Pain Syndrome are other conditions that are included under the umbrella term of Persistent Pelvic Pain. Some persistent pelvic pain conditions have no known cause. Physiotherapists are often part of an inter-disciplinary team assisting people with persistent pelvic pain to reduce symptoms and improve function. This may include pelvic floor muscle down-training, breathing and relaxation exercises or vaginal dilators/trainers.

Sexual Dysfunction
Pain with intercourse is not normal. Determining the driving factors is important to resolve symptoms. Pelvic health physios are uniquely qualified to assess and treat this cohort of people. We can also link in with appropriate Psychologists and/or Counsellors when needed.
Types of Pelvic Health Physiotherapy Services

Pre and Post Surgery
Prostatectomy: prepping the pelvic floor muscles correctly before surgery can drastically reduce time to regaining continence after prostate surgery
Bowel surgeries: rehabilitation to promote long term healthy bowel habits and control
Urogynaecological surgeries: pre-surgical advice and education to optimise your recovery; rehabilitation to optimise surgical results and promote long term healthy bladder habits and control.
Breast cancer surgery: regaining normal shoulder and upper limb function, safe exercise guidance and prescription, screening for lymphoedema and cording.

Antenatal and Postnatal
Physiotherapy education throughout the pregnancy regarding posture, normal bodily changes, and the role of the abdominal and pelvic floor muscles including appropriate exercise prescription. We also help the mother prepare for birth and can treat common pregnancy-related low back pain and pelvic girdle pain. We recommend routine follow-up after delivery (regardless of mode of delivery) to ensure optimal return to function, exercise and sport. The use of real-time ultrasound can help measure any abdominal muscle separation (rectus abdominis diastasis), track its improvement and allow feedback from the core muscles to ensure they are working effectively.
Pessary Fittings
For those patients with symptomatic prolapse, unrelieved by pelvic floor muscle training alone, a pessary can be lifechanging. A pessary is a device (made of medical grade silicone) that is fitted and worn inside the vagina. It should be comfortable and pain-free. It should not cause any complications; in fact, it should relieve the symptoms of prolapse and allow fuller participation in activities of daily living and exercise.
What I Can Expect From Pelvic Health Physiotherapy Sessions
Pelvic Health Physiotherapists spend time with their patients taking an extensive history of your story, symptoms and the impact of your condition on your life and well being. For best care they need to understand how your symptoms impact you as an individual. Following the subjective exam, a physical assessment may involve the following:
Real time ultrasound imaging
On the abdomen (tummy) to measure:
- Abdominal separation
- Core muscle activation, coordination and control
- Bladder volume pre and post void
- Pelvic floor muscle ability to lift bladder
On the perineum (tissue between the vagina and anus on females, tissue between scrotum and penis on males) to measure:
- Pelvic floor muscle endurance, repetitions, elevation and timing
- Bladder movement on coughing
External visual observation of the perineum
External visual observation of the perineum is useful for:
- Tissue health
- Movement of the tissues with pelvic floor muscle contractions and relaxations
- Movement of the tissues on coughing and straining
Internal vaginal examination
Internal vaginal examination is useful for:
Full pelvic floor muscle examination
- Tension in the muscles
- Function (including strength, endurance and coordination)
- Pain response
Prolapse examination
Digital rectal examination
Digital rectal examination is useful for:
- Assessing strength of anal sphincter muscle
- Assessing coordination of emptying technique
For a complete assessment, a digital vaginal and/or rectal examination is proposed. This examination helps to identify to what extent your pelvic floor muscles contribute to your problem/s, and also helps the Physiotherapist to prescribe the more effective treatment for you based on examination findings.
The Physiotherapist will explain what happens during the examination. You will be given time to consider whether to have this examination or not, and also to ask questions about the procedure. You have the right to make clear anything that you do not understand without feeling rushed about your decision.
You do not have to have an internal examination if you do not want it. The Physiotherapist will offer you alternative ways to examine or not examine your pelvic floor muscles. The Physiotherapist can still continue the treatment; however, the treatment may not be as beneficial as the treatment you have following the internal examination.
There should be no pain during the examination and if you are in pain, it is important to report it to the Physiotherapist. In general, if you are bothered by pain or in any other way during the examination, please tell your Physiotherapist at the time.
This section comes from the Patient Consent Form for Internal Examination – Acknowledgements RPH created by Irena Nurkic for Curtin